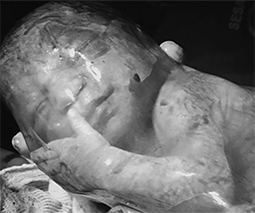
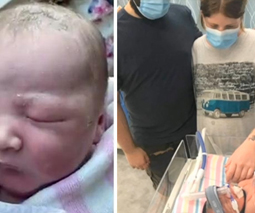
Birth story: How I coped when my ‘birth plans’ went awry

My first pregnancy was classified as ‘high risk’, with elevated blood pressure and gestational diabetes. Still, the majority of my pregnancy was relatively straightforward and uneventful. That was, until week 37.
Although both my blood pressure and diabetes were borderline, I was monitored very closely. I didn’t require any extra tests or medical intervention but I took my blood pressure at home, I checked my sugars and my diet and exercise regime changed. I saw an endocrinologist and a diabetes nurse.
Of course, this meant that our birth plan was very much in the hands of the professionals.
When we first saw our obstetrician, while labour was preferred, we were all of the belief that whatever needed to happen to keep the baby and me safe was fine by us – including a caesarean section.
Our aim was to get beyond 36 weeks. Because of the elevated blood pressure, there was a high possibility that the baby would need to come early. For 36 weeks, my blood pressure remained stable. There were even times when it dropped below normal. Winning!
High blood pressure and a false alarm
At the end of week 37, my blood pressure reading came back sky high. The second and third readings (taken two and 30 minutes later) were also high. I called my obstetrician. The result: head to the hospital.
Off I went, advising my husband to be on call should the doctors decide it was time. I was monitored for a few hours and, luckily, sent home. All was right with the world again.
But it did give us a very big scare.
Getting ready for induction
At our next appointment with our obstetrician, the decision was made to get the baby out to avoid him going into distress.
Imagine my husband’s face when our doctor said he’d see if he could get us in that night. White as a feather!
Rather than surgery, and under our doctor’s advice, we chose induction. We were still aiming for a vaginal delivery. By 10pm Saturday night I had been induced.
By morning, I had endured three unsuccessful and very painful attempts to break my waters. That was when the anaesthetist arrived. My lovely, caring, unbelievable obstetrician said if they were going to put me through that kind of pain again, I wasn’t going to feel it.
Following the fourth attempt, despite not feeling anything, the machine next to me said I was having strong contractions about 10 minutes apart. We were well on our way.
Four hours later everything went haywire.
The decision to have an emergency caesarean
With our final check, there was still too much fluid around my baby and things were getting a tad too dangerous. For fear of us both going into distress, my doctor said in a very calm and encouraging voice that we’d meet our baby within the hour. I was being prepped for surgery.
The anaesthetist returned to top up my epidural and within 15 minutes he and my husband were wheeling me down to surgery. No time to wait for a porter!
Bright lights greeted us. There were nurses, a new midwife and a surgical assistant to meet, people talking, beds moving. Everything was happening very quickly and yet, despite being classified as an emergency caesarean section, everyone and everything was calm.
My husband held my hand, our anaesthetist narrated everything, the surgical assistant told me to take a big deep breath, there was a push on my tummy, a few tugs, and then heavenly newborn screams. Within minutes, my son was in my arms.
Dealing with a ‘failed’ birth plan – 5 things that helped
1. We tried (and failed) to sleep
Our night was very disruptive with midwife visits and hourly checks. So, we rested. Regardless of how this was going to go, we both needed as much energy as possible.
2. We talked about our little baby
We discussed names (because we still hadn’t decided on a boy’s name). We considered how our life was about to change. Talking kept our minds off everything that was happening; it gave us some control.
3. We kept our families updated
While some couples choose to keep quiet, and others tell the world, we kept it in the family. We texted and called to include them in our birth, meaning we could give them information without numerous phone calls coming through.
4. We listened
The incredible medical experts around us told us exactly what was happening and why. When they said to wait, we waited. When they said to take the gas, I took the gas … and then spat it out. We wholeheartedly put our trust in the team and because of that, we were calm. Nothing was unexpected and we were prepared.
5. We laughed
A lot! In fact, within the first hour of being admitted my husband had me in stitches by accidentally brushing his teeth with Deep Heat.
While an emergency caesarean section wasn’t the birth we imagined, things ended up fine.
Some women plan to give birth naturally and end up under general anaesthetic. Some think they’re going in for surgery but their babies just can’t wait.
At the end of the day, my little boy is here and I have a scar just above my pubic bone. Regardless of how he entered the world, he’s a happy little Vegemite who constantly gets into mischief. And isn’t that the most important thing of all?