I’m just going to say it: I wish I had an epidural

It seems there are two distinct camps when it comes to childbirth ideologies. There are the mothers who have natural, drug-free births, and at the other end of the scale, the mothers who elect to have epidurals.
What do they have in common?
Both camps proudly tell anyone within earshot why they made the decision to birth that way. In fact, I’d go so far as to say they wear their birthing method like a badge of honour.
The natural birthing mums
There’s a whole host of valid reasons behind their choice to birth without drugs. These relate to the way women’s bodies are physiologically designed to give birth, safety concerns around administering painkillers, unnecessary medical interventions and their potential effects on the baby, and of course, how empowering a natural birth can be. I’ve got to say, it feels a bit like an exclusive club, though.
The epidural mums
Their justification for pain relief typically has traces of defensiveness and self-deprecating cynicism. If the natural birthing mums are the perfect older sisters, getting straight-As on their childbirth assessment, then the ‘gimme all the drugs’, don’t-give-a-shit women are the rebellious younger sisters, trying as hard as they can to be different from their older sister.
Or at least that’s how it feels to me.
But what if you don’t fit either camp?
Then there’s the rest of us – the ones in between, the floaters – that either didn’t get to choose whether we had pain relief (perhaps because of an emergency c-section), or dabbled in some pain relief (gas or morphine) but didn’t commit to the full epidural effect.
We are the women whose day (and night!) of labour doesn’t say much about us as a person. Though it does help us decide which clump of mothers we’ll gravitate towards (and which mothers we’ll secretly scorn) at Mother’s Group.
My epidural-less birth
I have one child, a beautiful boy, whom I gave birth to four years ago. It was a fairly routine vaginal birth, and had no significant complications, other than the fact that like many first-time mothers, my baby took his sweet time arriving.
There was just one minor risk factor in my son’s position in utero, (it happens in 20 percent of first-time pregnancies.) He had what’s called a ‘high head’. Basically, his head wasn’t engaged in the pelvis or pressing on my cervix, sending a signal to my body that labour should start, and then progress.
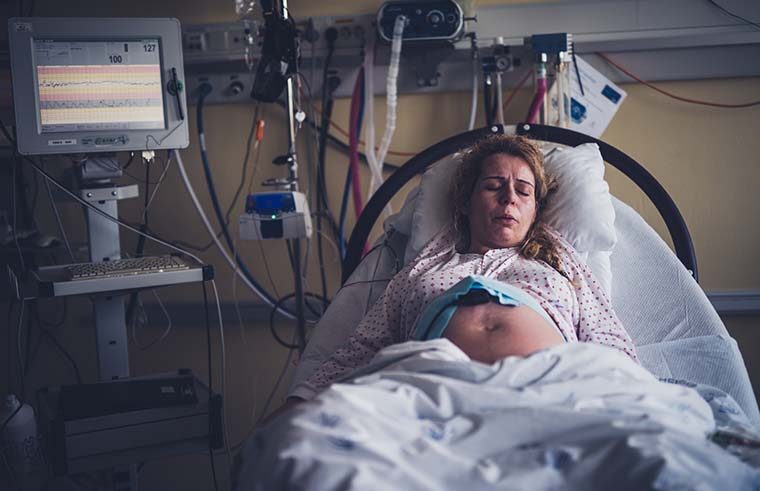
Why I wish I had an epidural (or at least seriously considered it)
I had intended on having as natural a birth as possible and had been practicing calm birthing techniques with my husband in the weeks leading up to my labour. My son arrived 11 days late, and by then I was over it.
During my last trimester, a few women I knew had given birth naturally.
As they told me their birth stories, I mistakenly thought that because they could cope with a natural birth, I could forgo the drugs too. They were a similar age, fitness level and body type. That’s all that mattered, right?
Wrong!
What I didn’t take into consideration was the fact that both of those women were induced for medical reasons at 38 weeks, and both had fairly short, five-hour labours.
Both women had babies whose heads were engaged weeks before they gave birth. And both women pushed out their baby boys in less than 15 minutes.
The factors that played in my son’s birth
I was in labour for just over 24 hours. I went into early labour at 9pm, and had steady contractions until we went to hospital at seven the next morning. During that time I found the calm birthing strategies worked for me (and my husband), at least for the first few hours.
But progress was slow because my son’s head still wasn’t engaged, I was only 2cm dilated when I got to hospital and exhausted from being up all night with contractions.
Instead of sending me home – a one-hour round trip – the hospital decided to give me an oxytocin drip to speed things along; essentially an induction. But I was never asked (to my knowledge) whether I wanted to be induced.
Perhaps I didn’t realise that’s what they were doing. I was so tired, I didn’t realise it was one of the ‘dreaded’ interventions that calm-birthing mothers are warned to avoid at all costs.
I continued to labour for another 15 hours, growing more and more exhausted with each contraction, and the fatigue made coping with the pain much harder. This was the factor women with shorter births don’t have to experience.
No two births can be compared
Here’s another unexpected factor. Because of a pre-existing childhood condition in my knees, I couldn’t kneel or sit on the floor and catch a brief moment of rest. I instinctively knew I didn’t want to lie down, especially when I felt a contraction coming on. I preferred to be upright, so I stood – at one point, for three hours straight!
Gas did nothing for me, only made me projectile vomit, all over the poor midwife.
I’d been so brave and so strong for so long, that, going almost 18 hours without any form of pain relief (besides a brief swig of gas) I finally moaned that I needed something. Morphine. An epidural.
But it was too late for an epidural because I was in transition. So they gave me morphine, which slowed down the baby’s progress again, but didn’t give me much respite.
I finally began pushing at 7pm – 22 hours into labour – and pushed for two long, gruelling hours. That’s eight times longer than my ’15 minute’ friends.
I wished I’d given into the pain
What was I so afraid of? Was it those glowing, Madonna-like, ‘perfect straight-A sisters’ and natural birthing Instagram mamas I imagined scorning me if I failed them? Why did I care so much about what they thought, or of how my birth would be judged when I told the story afterwards?
It was my birth. It was me in that labour room. And I should have known: I was the one who got to call the shots.
Just because she had a natural birth, doesn’t mean you should.
And equally, just because she had an epidural, doesn’t mean you should.
You should do exactly what you feel you need to do, and what your body and mind is telling you, based on the unique set of circumstances you find yourself in.
We’re in danger of believing that because it happens in a certain ‘ideal’ way for one woman, it will happen that way for us. And this doesn’t just apply to natural births. Not all women experience satisfactory relief from an epidural, so basing my decision to get an epidural on another mother’s experience was also unwise.
Two camps aren’t enough when it comes to childbirth
There should be millions of camps, not just two, because no two women experience the same feelings, emotions, physical sensations, pain, and effectiveness of pain relief during birth.
The reality is that there are so many factors that influence a labouring woman’s decision whether or not to accept pain relief. But none of these factors should include the choices her friend, sister or natural birthing Instagram community made.
If you, or someone you know has experienced a traumatic birth, help is available. Go to birthtrauma.org.au or call Lifeline: 13 11 14