Measles 101: A family guide to measles

As immunisation rates fall, measles is rearing its ugly head again, here’s what you need to know about this serious, wildly infectious virus.
Measles 101
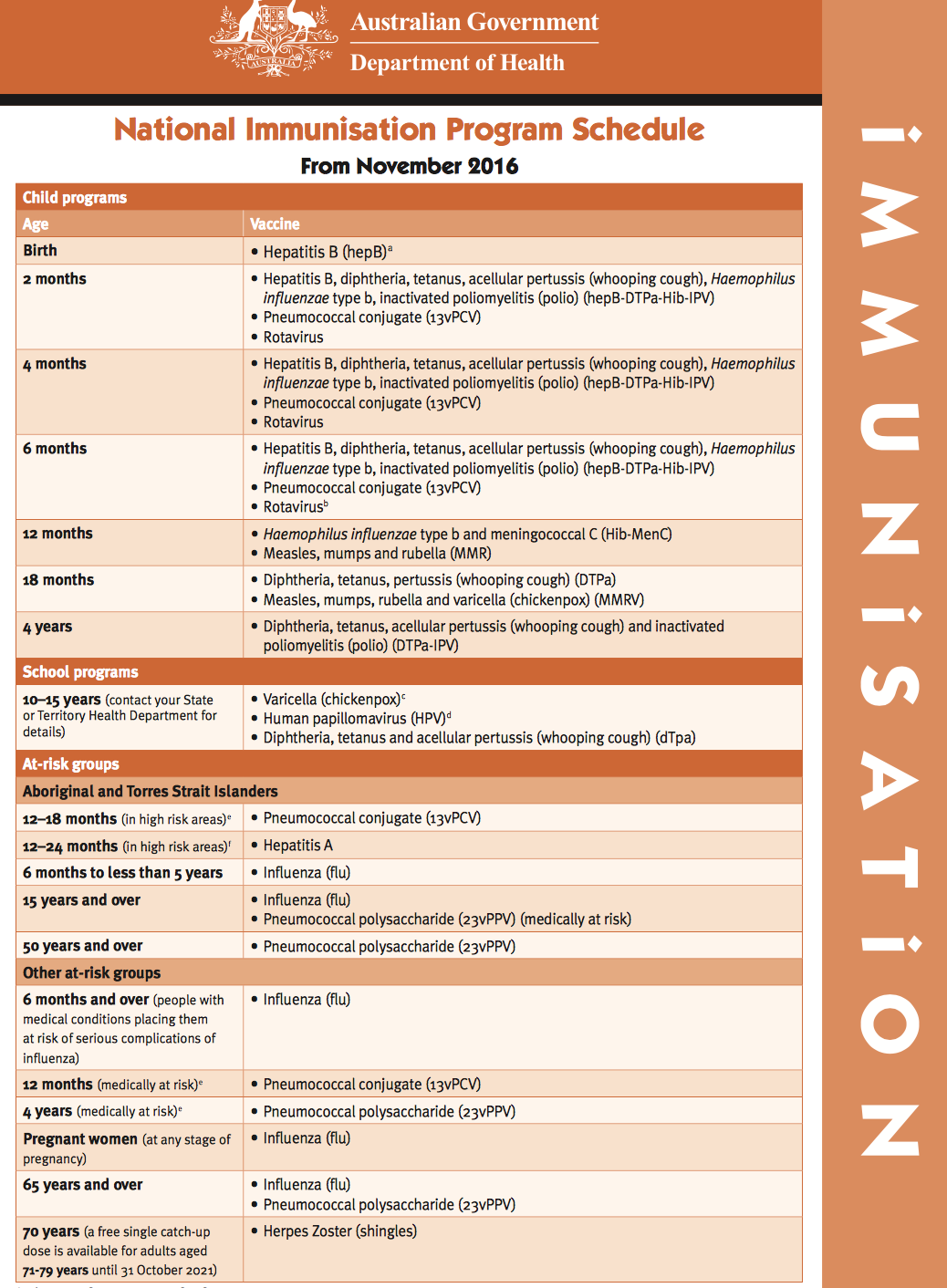
MMR and MMRV vaccinations
Measles symptoms
- fever
- loss of appetite
- general discomfort or feeling unwell
- runny nose
- diarrhoea
- dry cough
- sore, red eyes
- sore ears
- red and bluish spots inside the mouth (known as Koplik’s spots)
- red and blotchy skin rash that appears first on the face and hairline, and then spreads to the body. The rash is not itchy.
Measles diagnosis and reporting
If a patient is showing symptoms of measles, a blood test and samples from the nose, throat and urine are collected to properly confirm the diagnosis.
In Australia, measles is a notifiable condition due to public health concerns. Doctors, hospitals and laboratories, schools and childcare centres must notify cases of measles to their local public health unit.
Measles exclusion
The incubation period for measles is approximately 10 days, but may range from 7 to 18 days from exposure to the onset of fever. It is usually 14 days until the rash appears.
Patients with measles should be isolated for at least 4 days after the rash begins.
Non-immunised people who have been in contact with someone with measles should be excluded until 14 days after the first day of appearance of rash in the last case.
If unimmunised contacts are vaccinated within 72 hours of their first contact with the first case, or if they receive immunoglobulin within 144 hours of the contact, they may return to school.
Measles complications
- inflammation of the middle ear
- diarrhoea and/or vomiting
- dehydration
- respiratory infections like bronchitis, croup or laryngitis
- pneumonia
- encephalitis
- subacute sclerosing panencephalitis (SSPE)
What to do if you think your child has measles
Protecting your baby from measles if they’re too young to be vaccinated
Check your own immunisation status is up to date, as well as the status of those in contact with the baby.
The optimal way to protect young babies from measles is to ensure that those in close contact with the baby are immunised.
If you are fully immunised for measles your baby will have received some immunity from you during pregnancy. If you are unsure, you can have a blood test to check if you are immune to measles. Have a chat to your GP about your concerns.
2017: Measles in Australia
Measles deaths worldwide
The World Health Organisation reports that:
- Measles is one of the leading causes of death among young children even though a safe and cost-effective vaccine is available.
- In 2015, there were 134 200 measles deaths globally – about 367 deaths every day or 15 deaths every hour.
- Measles vaccination resulted in a 79 per cent drop in measles deaths between 2000 and 2015 worldwide.
- In 2015, about 85 per cent of the world’s children received one dose of measles vaccine by their first birthday through routine health services – up from 73 per cent in 2000.
- During 2000-2015, measles vaccination prevented an estimated 20.3 million deaths making measles vaccine one of the best buys in public health.









